Best antibiotic for tooth infection sets the stage for this crucial discussion, exploring the various treatment options available for tooth infections. From understanding the importance of timely antibiotic treatment to managing antibiotic resistance, this guide will delve into the key considerations for effectively treating tooth infections.
With millions of people worldwide affected by tooth infections, finding the best antibiotic for tooth infection has become increasingly important. This guide will walk readers through the various types of tooth infections, including periapical, dentoalveolar, and periodontal infections, and discuss the antibiotics commonly used to treat these infections.
Classification of Tooth Infections and Suitable Antibiotics

Tooth infections are a common dental issue that can cause significant pain and discomfort. These infections can be classified into three main categories: periapical, dentoalveolar, and periodontal infections. Each type of infection has distinct characteristics and treatment options.
Periapical Infections, Best antibiotic for tooth infection
Periapical infections occur at the tip of a tooth’s root, often as a result of a cavity or a cracked tooth. This type of infection can cause severe pain and swelling in the surrounding gum and bone tissue. Common antibiotics used to treat periapical infections include:
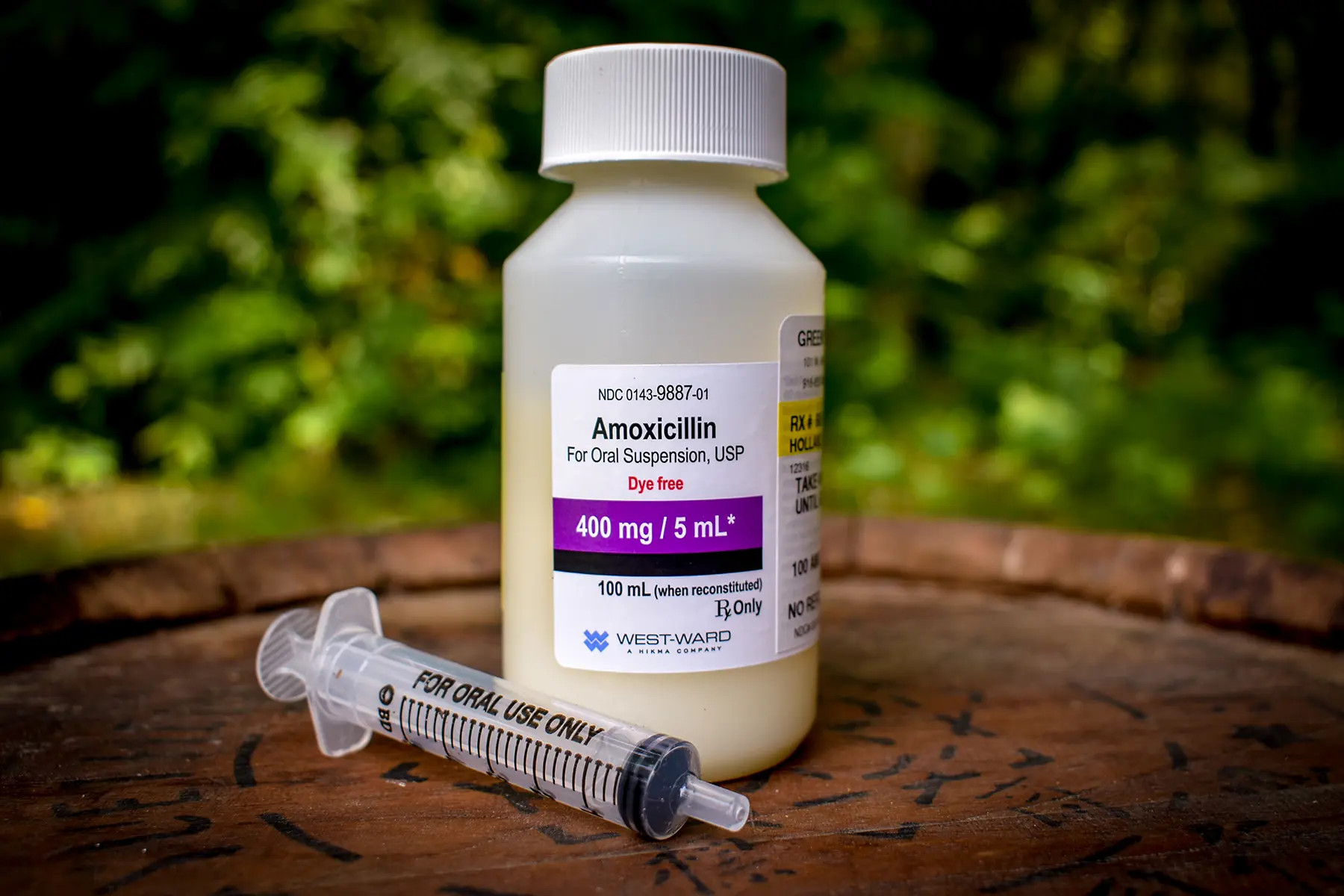
- Amoxicillin: This broad-spectrum antibiotic is often the first choice for treating periapical infections. It targets a wide range of bacteria, including Streptococcus and Staphylococcus species.
- Clindamycin: This antibiotic is also effective against periapical infections, especially when amoxicillin is not tolerated. It is particularly useful for patients with penicillin allergies.
- Metronidazole: This antibiotic is used to treat periapical infections caused by anaerobic bacteria, such as Bacteroides and Fusobacterium species.
Dentoalveolar Infections
Dentoalveolar infections occur in the tissue surrounding a tooth, often as a result of a dental procedure or trauma. This type of infection can cause pain, swelling, and bleeding in the affected area. Common antibiotics used to treat dentoalveolar infections include:
- Cephalexin: This oral antibiotic is effective against dentoalveolar infections caused by Streptococcus and Staphylococcus species.
- Cephazolin: This intravenous antibiotic is used to treat severe dentoalveolar infections, particularly in patients with compromised immune systems.
- Azithromycin: This antibiotic is used to treat dentoalveolar infections caused by Gram-negative bacteria, such as E. coli and Klebsiella species.
Periodontal Infections
Periodontal infections occur in the supporting structures of the tooth, including the gum and bone tissue. This type of infection can cause pain, bleeding, and swelling in the affected area. Common antibiotics used to treat periodontal infections include:
- Metronidazole: This antibiotic is used to treat periodontal infections caused by anaerobic bacteria, such as Bacteroides and Fusobacterium species.
- Amoxicillin: This broad-spectrum antibiotic is often used to treat periodontal infections, particularly when combined with metronidazole.
- Tetracycline: This antibiotic is used to treat periodontal infections caused by Gram-positive bacteria, such as Staphylococcus and Streptococcus species.
Natural Antibiotic Alternatives for Tooth Infections

Tooth infections can be a real pain, and while antibiotics are often the go-to solution, some people may prefer to try natural alternatives. These can be an effective way to combat tooth infections, and they often come with fewer side effects and risks compared to traditional antibiotics.
As we explore natural antibiotic alternatives for tooth infections, keep in mind that while these options can be effective, they may not work as quickly as antibiotics and might require repeated application or use over a longer period. Always consult with a dentist or healthcare professional before trying any new remedies, especially if you have a severe tooth infection or are at risk of complications.
Essential Oils and Tooth Infections
Some essential oils have been studied for their antibacterial properties and potential to combat tooth infections. For example:
- Tea tree oil (Melaleuca alternifolia) has been shown to inhibit the growth of certain bacteria that can cause tooth infections. Studies have used diluted tea tree oil applied directly to the affected area or as a mouthwash. However, more research is needed to confirm its effectiveness.
- Oregano oil (Origanum vulgare) has demonstrated antimicrobial properties against Streptococcus mutans, a bacteria commonly associated with tooth decay and infections.
- Thymus oil (Thymus vulgaris) has been researched for its ability to combat periodontal infections and reduce inflammation.
Remember to use high-quality essential oils that are pure and have not been mixed with other substances. Always dilute essential oils in a carrier oil before applying them to your skin or gums, and follow proper usage guidelines to avoid irritation or allergic reactions.
Herbal Remedies for Tooth Infections
Certain herbs may help alleviate symptoms and prevent tooth infections by promoting oral health. Some examples include:
- Ginger (Zingiber officinale) has anti-inflammatory properties that can help reduce pain and swelling associated with tooth infections.
- Garlic (Allium sativum) has been studied for its antimicrobial properties and potential to combat periodontal infections.
- Goldenseal (Hydrastis canadensis) has been used to treat oral infections due to its antimicrobial properties.
Keep in mind that while these herbs may help reduce symptoms, they may not eliminate the underlying infection. Consult with a healthcare professional before using herbal remedies, especially if you have a severe tooth infection or are taking medications that may interact with the herbs.
Effective Dosage and Duration of Antibiotic Treatment for Tooth Infections: Best Antibiotic For Tooth Infection
When it comes to treating tooth infections with antibiotics, it’s not just about taking the right medication, but also ensuring you’re taking it for the right amount of time. Overlooking the dosage and duration can lead to treatment failure, worsening of the infection, and even the development of antibiotic-resistant bacteria. Completing the full course of antibiotic treatment is crucial to achieve the best possible outcome for your tooth infection.
Dosing Guidelines for Common Tooth Infections
The choice of antibiotic and dosage depends on the type and severity of the tooth infection, as well as the patient’s overall health. Here are some general guidelines for common tooth infections:
Mild to Moderate Tooth Abscess
For mild to moderate tooth abscesses, the recommended antibiotic treatment is typically a combination of amoxicillin and clavulanic acid (Augmentin) or amoxicillin (Amoxil). The dosing guidelines for these antibiotics are as follows:
- Amoxicillin and Clavulanic Acid: 500mg-875mg orally, every 8 hours for 5-7 days.
- Amoxicillin: 500mg-1g orally, every 8 hours for 5-7 days.
It’s essential to note that these dosing guidelines may vary depending on the severity of the infection and the patient’s overall health.
Severe Tooth Abscess
For severe tooth abscesses, the recommended antibiotic treatment may involve stronger antibiotics such as clindamycin (Cleocin) or metronidazole (Flagyl). Dosing guidelines for these antibiotics are as follows:
- Clindamycin: 150mg-450mg orally, every 6 hours for 5-7 days.
- Metronidazole: 250mg-500mg orally, every 6 hours for 5-7 days.
As with mild to moderate infections, these dosing guidelines may vary depending on the severity of the infection and the patient’s overall health.
Antibiotic Treatment Duration
It’s essential to complete the full course of antibiotic treatment to ensure the infection is fully eradicated and to prevent relapse. Stopping the antibiotics prematurely can lead to treatment failure and worsening of the infection. A minimum of 5-7 days of antibiotic treatment is recommended, with some cases requiring longer treatment durations.
The American Dental Association recommends completing the full course of antibiotic treatment to ensure optimal outcome and prevent antibiotic resistance.
Follow-up Care
After completing the antibiotic treatment, it’s essential to schedule a follow-up appointment with your dentist to ensure the infection has resolved and to address any remaining dental needs. Your dentist may perform a follow-up examination to confirm the infection has cleared and to provide guidance on any further dental care or treatments.
Final Conclusion
The best antibiotic for tooth infection will depend on the severity and type of infection, as well as individual factors such as age, medical history, and allergies. By understanding the causes and symptoms of tooth infections, and choosing the right antibiotic treatment, patients can feel empowered to take control of their oral health. In conclusion, with the right approach, tooth infections can be effectively treated, and a healthy smile maintained.
Query Resolution
Q: What are the most common antibiotics used to treat tooth infections?
A: The most common antibiotics used to treat tooth infections include amoxicillin, penicillin, and clindamycin.
Q: Can I get a tooth infection from biting my tongue or cheek?
A: While biting your tongue or cheek can cause temporary pain and discomfort, it is unlikely to cause a tooth infection.
Q: How long does it take for antibiotics to work on a tooth infection?
A: Antibiotics can take anywhere from a few days to a week to start working on a tooth infection, depending on the severity of the infection and the type of antibiotic used.
Q: Can I use natural remedies to treat a tooth infection?
A: While natural remedies such as essential oils and herbal extracts can be used to help manage the pain and discomfort associated with a tooth infection, they may not be effective in completely treating the infection.
Q: How do I know if I have a tooth infection?
A: Symptoms of a tooth infection can include severe toothache, swelling, and sensitivity to hot or cold temperatures, as well as pain when biting or chewing. If you experience any of these symptoms, it is essential to visit a dentist as soon as possible.