Best birth control sets the stage for comprehensive birth control information, offering readers a well-rounded view of various methods, from hormonal and barrier control to natural and emergency contraception. It tackles topics such as menstrual regulation, hormonal balance, and safe sex practices, providing a foundation for an in-depth exploration of birth control options.
Discussing different types of birth control, including combined hormonal methods, hormonal IUDs, progesterone-only pills, condoms, fertility awareness methods, IUDs, and natural products, the article highlights the benefits and drawbacks of each, giving readers a clear understanding of the available choices. It emphasizes the importance of safe sex practices and access to affordable healthcare, making a compelling case for birth control accessibility.
Different Types of Birth Control Methods for Managing Hormonal Imbalance
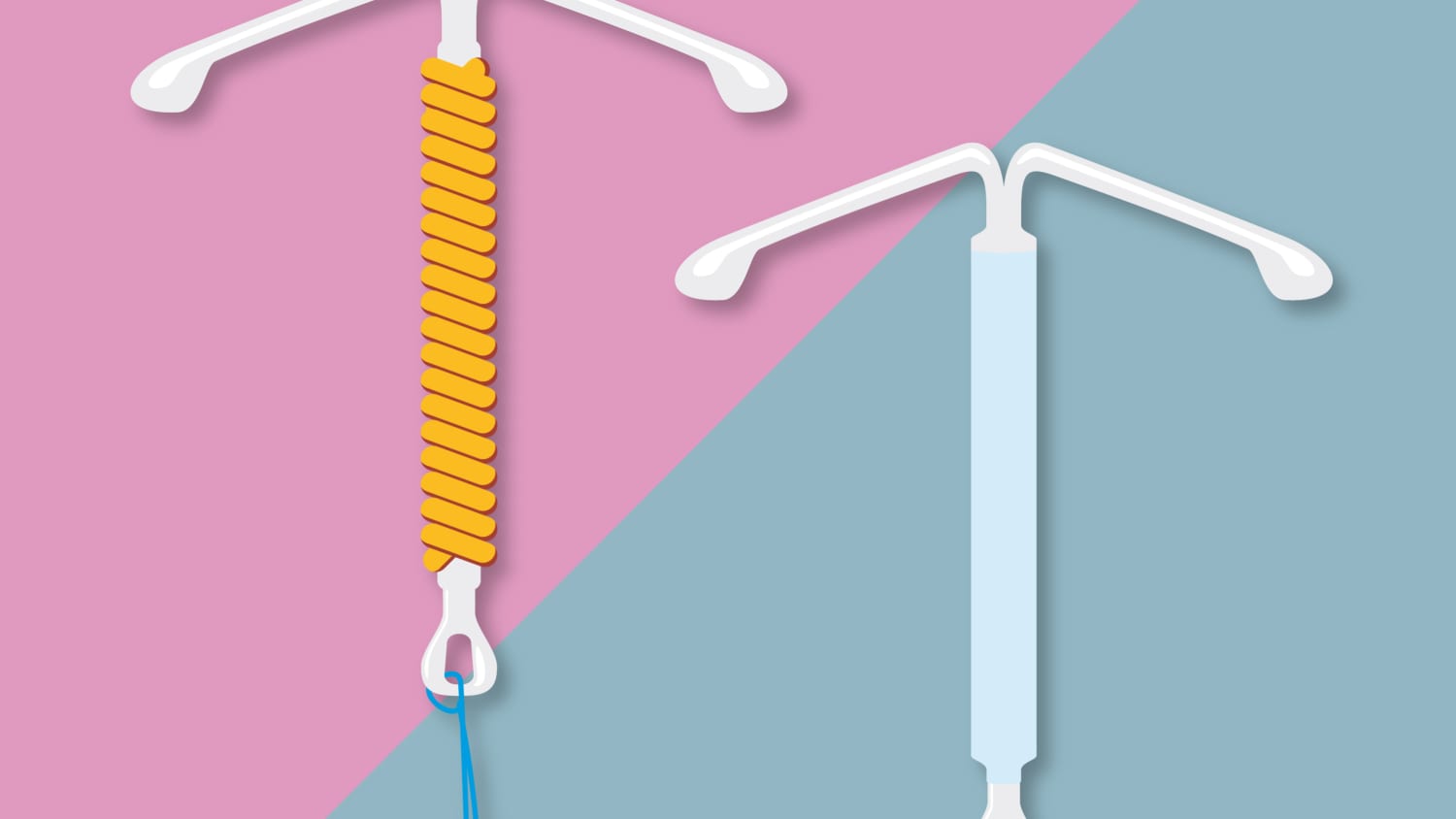
Birth control methods have become an essential aspect of reproductive health, particularly for managing hormonal imbalances. Hormonal imbalances can lead to a range of issues, including irregular menstrual cycles, polycystic ovary syndrome (PCOS), and increased risk of certain cancers. Effective management of hormonal imbalances requires the right birth control method, tailored to an individual’s specific needs.
Combined Hormonal Birth Control Methods, Best birth control
Combined hormonal birth control methods, such as the combined pill, patch, and vaginal ring, work by releasing both estrogen and progesterone hormones into the body. This combination helps regulate menstrual cycles, leading to a more predictable and manageable period. According to a study published in the Journal of Clinical and Translational Research, the use of combined hormonal birth control methods can reduce menstrual cramps, heavy bleeding, and mood swings in women with hormonal imbalances.
- Regulation of menstrual cycles: The combined pill, patch, and vaginal ring can help regulate menstrual cycles, reducing the frequency and severity of menstrual cramps.
- Reduction of heavy bleeding: The estrogen in these methods helps regulate blood flow, reducing the risk of heavy bleeding during periods.
- Mood stabilization: The progesterone in these methods can help stabilize mood, reducing the risk of anxiety and depression in women with hormonal imbalances.
However, these methods are not ideal for women who are prone to blood clots or have a history of certain medical conditions, such as liver disease or high blood pressure.
Hormonal IUDs
Hormonal intrauterine devices (IUDs) are a long-term reversible contraceptive method that release progestin hormones into the body. These hormones work by thickening the cervical mucus, preventing sperm from reaching the egg, and also thinning the uterine lining to prevent implantation of a fertilized egg. According to a study published in the British Journal of Obstetrics and Gynaecology, hormonal IUDs can reduce menstrual bleeding by up to 90% and also reduce the risk of ovarian and endometrial cancers.
- Reduction of menstrual bleeding: Hormonal IUDs can significantly reduce menstrual bleeding, making it an ideal option for women with heavy periods.
- Effective contraception: Hormonal IUDs are one of the most effective forms of contraception, with a success rate of over 99%.
- Long-term reversible: Hormonal IUDs are a long-term reversible method, making them an ideal option for women who want a permanent form of birth control but want the option to reverse it in the future.
However, hormonal IUDs are not suitable for women with a history of pelvic inflammatory disease (PID), and there is a small risk of expulsion or perforation of the uterus during insertion.
Progesterone-only Birth Control Pills
Progesterone-only birth control pills, also known as mini-pills, work by releasing only progesterone hormones into the body. These hormones work by thickening the cervical mucus, preventing sperm from reaching the egg, and also preventing ovulation in the majority of women. According to a study published in the Journal of Clinical and Translational Research, progesterone-only birth control pills can reduce menstrual bleeding, making them an ideal option for women with PCOS.
- Reduction of menstrual bleeding: Progesterone-only birth control pills can significantly reduce menstrual bleeding, making them an ideal option for women with heavy periods.
- Effective contraception: Progesterone-only birth control pills are effective in preventing pregnancy.
- Potential benefits for women with PCOS: Progesterone-only birth control pills have been shown to have potential benefits for women with PCOS, including reduced acne and improved insulin sensitivity.
However, these pills must be taken at the same time every day to be effective, and there is a small risk of breakthrough bleeding or spotting.
It is essential to consult a healthcare provider before choosing a birth control method, as they can help determine the best option based on individual needs and medical history.
Safe and Effective Birth Control Options for Young Adults: Best Birth Control

For young adults, choosing the right birth control method can be a daunting task. With numerous options available, it’s essential to understand the advantages and disadvantages of each method to make an informed decision. One popular barrier method of birth control for young adults is condoms, which not only prevent unintended pregnancies but also reduce the risk of sexually transmitted infections (STIs).
Advantages and Disadvantages of Condoms as a Barrier Method
Condoms are a widely used and accessible form of birth control, and they offer several advantages. They are inexpensive, easily available, and non-hormonal, making them a great option for those who prefer not to use hormonal birth control. Condoms are also a convenient method, as they can be used for both vaginal and anal sex. Additionally, they provide a sense of protection and control for young adults, which can be empowering.
However, condoms also have some disadvantages. They can reduce the intensity of orgasm and may cause allergies or irritation in some individuals. Furthermore, if used incorrectly or consistently, they can fail to prevent unintended pregnancies or STIs. The failure rate for condoms is around 2-18% when used consistently and correctly, but it can be much higher if not used properly (Source: CDC).
Importance of Proper Condom Use and Maintenance
Proper condom use and maintenance are crucial to prevent unintended pregnancies and STIs. This includes using condoms consistently and correctly, storing them properly, and checking the expiration date before use. It’s also essential to choose condoms that fit correctly and are made from latex or polyurethane, as these materials are more effective at preventing STIs (Source: Planned Parenthood).
When using condoms, it’s essential to follow proper application and removal techniques. This includes placing the condoms on the penis before any genital contact and removing them carefully after ejaculation. Additionally, it’s crucial to check for any signs of damage or expiration before use, as damaged or expired condoms can increase the risk of STIs and unintended pregnancies.
Preventing STIs through Condom Use
In addition to preventing unintended pregnancies, condoms can also help prevent the transmission of STIs. This is because condoms create a physical barrier that prevents the exchange of bodily fluids, which can contain STIs. However, it’s essential to note that condoms are not 100% effective in preventing STIs, and other forms of birth control, such as hormonal methods or vaccines, may be necessary for complete protection.
To maximize the effectiveness of condoms in preventing STIs, it’s essential to use them consistently and correctly, as well as get regular STI testing and treatment if necessary. This can include regular check-ups with a healthcare provider, as well as getting vaccinated against HPV and other STIs (Source: CDC).
Comparing Emergency Contraception Options for Preventing Unintended Pregnancies
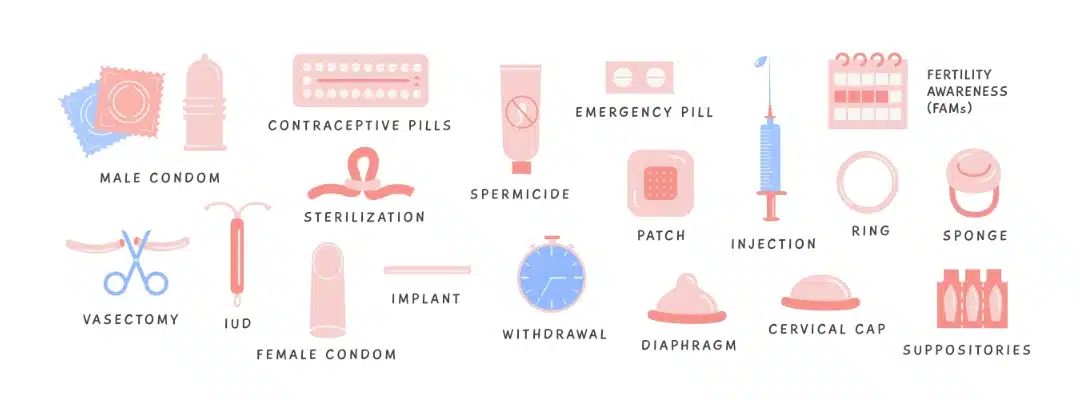
Emergency contraception serves as a safeguard against unintended pregnancies. However, with various options available, it’s crucial to understand the efficacy and duration of protection offered by each. This understanding enables informed decision-making and responsible use of emergency contraception.
Efficacy and Duration of Protection: Plan B vs. Ella
Plan B and Ella are two widely used emergency contraceptives. Both can prevent unintended pregnancies when taken within specific timeframes. Plan B, also known as the ‘morning-after pill,’ contains 1.5 mg of levonorgestrel and is designed for individuals who missed a regular birth control pill or experienced unprotected sex. Its efficacy in preventing pregnancy is highest when taken within 72 hours after intercourse. According to the CDC, Plan B is 95% effective when taken within 24 hours and 89% effective when taken within 3 days.
However, its effectiveness decreases over time, reaching 58% efficacy when used beyond 72 hours.
On the other hand, Ella, also known as ulipristal acetate, offers longer-lasting protection, with a 98% efficacy rate when taken within 120 hours (5 days) after intercourse. It’s available in a single, 30-mg dose.
- Plan B (levonorgestrel): 1.5 mg, 80-89% effective within 3 days, 95% effective within 24 hours
- Ella (ulipristal acetate): 30 mg, 98% effective within 120 hours (5 days)
The choice between Plan B and Ella depends on individual circumstances and personal preferences. For those with a history of irregular periods or hormone-sensitive conditions, Ella may be a safer option. Conversely, Plan B is often the preferred choice for those with no known allergies or contraindications.
Importance of Seeking Medical Attention After Taking Emergency Contraception
In addition to choosing the right emergency contraceptive, understanding the importance of post-treatment medical evaluation is crucial. If symptoms persist or worsen, such as vaginal bleeding, heavy menstrual periods, or abdominal pain, medical attention should be sought promptly. Early intervention can help address underlying health issues and prevent prolonged discomfort.
It is essential to note that emergency contraception does not offer ongoing birth control protection; a regular birth control method should be resumed as soon as possible.
Wrap-Up
In conclusion, best birth control emphasizes the significance of birth control in managing hormonal balance, preventing unintended pregnancies, and reducing the risk of STIs. By shedding light on the various available options, the article empowers readers to make informed decisions about their reproductive health and encourages discussion around affordable healthcare access.
User Queries
What is the most effective form of birth control?
The most effective form of birth control is the intrauterine device (IUD), which has a failure rate of less than 1%. However, the method of choice ultimately depends on individual preferences and needs.
Can I use birth control if I’m breastfeeding?
Yes, most birth control methods are safe to use while breastfeeding, but it’s essential to consult with a healthcare provider to determine the best option for your individual situation.
What is the difference between Plan B and Ella?
Plan B and Ella are both emergency contraceptives, but they work in different ways and have slightly different efficacy rates. Ella, also known as ulipristal acetate, is more effective and has a longer window of use.
Can I use natural birth control methods if I have PCOS?
Natural birth control methods, such as the fertility awareness method (FAM), may be suitable for women with PCOS, but it’s essential to monitor ovulation and use additional methods, like a backup plan, to maintain effectiveness.
Are condoms effective in preventing STIs?
Yes, condoms are highly effective in preventing STIs, including HIV, when used correctly and consistently, but no method is 100% effective, and other methods of protection, like regular testing and vaccinations, should be considered.
How do I choose the best birth control method for me?
It’s essential to consult with a healthcare provider to discuss your individual needs, preferences, and health status. They will help you determine the best birth control method, considering factors like hormonal balance, menstrual regulation, and STI prevention.