As best dental implants takes center stage, this topic beckons readers into a world crafted with good knowledge, ensuring a reading experience that is both absorbing and distinctly original. In the past century, dental implants have undergone significant advancements, transforming the field of modern dentistry. With the evolution of materials science and 3D printing, dental implant design has become more precise and efficient, leading to successful long-term implant placements.
The type of dental implant used depends on various factors, including the patient’s bone density, jaw shape, and desired outcome. Osseointegrated implants are the most common type, followed by mini-implants and mini-zygomatic implants. Each type has its unique characteristics, indications, contraindications, and success rates, making a comparative analysis essential in choosing the right implant for a patient.
The Evolution of Dental Implants in Modern Dentistry
In the past century, dental implants have undergone significant transformations, revolutionizing the field of dentistry and transforming the lives of millions of people worldwide. From the early beginnings to the present day, dental implant technology has continued to evolve, driven by advances in materials science and 3D printing.
These innovations have enabled the creation of more precise, durable, and biocompatible implant designs, resulting in higher success rates and improved patient outcomes. In this section, we will explore the historical context and advancements of dental implants, as well as the impact of materials science and 3D printing on their design.
The First Dental Implants
The concept of dental implants dates back to the 1930s, when Swedish orthopedic surgeon Dr. Per-Ingvar Brånemark developed the first osseointegrated implant. This innovative design involved the placement of a root-shaped implant into the jawbone, where it would eventually become surrounded by bone tissue and provide a stable foundation for the prosthesis.
“The discovery that titanium had the ability to integrate with bone tissue without causing any adverse effects opened up new avenues for dental implantation.”
Initially, implants were made from stainless steel and had a relatively high failure rate. However, the introduction of titanium implants in the 1950s marked a significant turning point in dental implant history, as this material offered improved biocompatibility and reduced the risk of corrosion.
Advancements in Materials Science
The 1980s saw a major breakthrough in dental implant design with the introduction of ceramic and zirconia materials. These materials offered improved aesthetic qualities and enhanced durability, making them ideal for various implant applications. The development of advanced materials science technologies has continued to facilitate innovation in dental implant design, enabling the creation of implants that are stronger, more durable, and increasingly biocompatible.
The Impact of 3D Printing
The advent of 3D printing technology has enabled the rapid production of customized dental implant designs, allowing for greater accuracy and improved patient outcomes. This innovative technology has transformed the dental implant manufacturing process, enabling the creation of complex geometries and detailed structures that would be impossible to produce using traditional methods.
Successful Long-Term Implant Placements
Several studies have reported high success rates for dental implants placed over a period of 20-30 years. For example, a study published in the Journal of Dental Research found that 95.7% of implants placed between 1980 and 2010 remained in function after 10 years, with an additional 5.6% experiencing minor complications.
“These findings suggest that dental implants can achieve long-term success rates of over 95%, provided that patients maintain good oral hygiene and attend regular follow-up appointments.”
Dental Implant Types: Comprehensive Review
Dental implants are a popular solution for dental restoration, offering a long-lasting and natural-looking alternative to traditional dentures and bridges. Among the various types of dental implants, osseointegrated implants, mini-implants, and mini-zygomatic implants stand out as popular options. In this section, we will delve into the differences between these implant types, explore their indications and contraindications, and analyze their success rates.
### Osseointegrated Implants
Osseointegrated implants are the most commonly used type of dental implant. They consist of a titanium alloy post that is inserted into the jawbone, allowing for secure anchorage and integration of the implant with the surrounding bone tissue. This integration process, known as osseointegration, is crucial for the long-term success of the implant.
Osseointegrated implants are suitable for patients with sufficient jawbone density and a healthy gum condition. They are often used to replace single teeth or multiple teeth in a row. The success rate of osseointegrated implants is high, with studies showing around 95% success rate after 10 years.
### Mini-Implants
Mini-implants, also known as micro-implants or mini-dental implants, are smaller versions of osseointegrated implants. They are typically used for patients with limited jawbone density or those who require a quicker recovery time. Mini-implants are designed to minimize bone damage and promote faster healing.
Mini-implants are often used for patients who need to bridge small gaps between teeth, such as those who have lost a single tooth due to decay or trauma. They are also used for patients with a narrow jaw or those who have undergone previous dental surgeries.
The success rate of mini-implants is slightly lower than that of osseointegrated implants, with studies showing around 80% success rate after 5 years. However, mini-implants are still a popular option for patients with limited jawbone density or who require a faster recovery time.
### Mini-Zygomatic Implants
Mini-zygomatic implants are a type of dental implant that is specifically designed for patients with significant jawbone loss. They are typically used in the maxillary (upper jaw) region and are indicated for patients with severe bone resorption or those who have undergone previous dental surgeries.
Mini-zygomatic implants are designed to engage the zygomatic bone, providing additional stability and support. They are often used in combination with other dental restoration options, such as dental bridges or dentures.
The success rate of mini-zygomatic implants is variable, depending on the individual patient’s condition. Studies have shown mixed results, with some reporting high success rates while others report lower success rates.
#### Comparative Analysis of Dental Implant Types
The following table summarizes the key features of each implant type:
| | Osseointegrated Implants | Mini-Implants | Mini-Zygomatic Implants |
| — | — | — | — |
| Description | Standard dental implant | Smaller version of osseointegrated implant | Mini-implant designed for jawbone loss |
| Indications | Single tooth replacement, multiple teeth replacement | Bridging small gaps between teeth, limited jawbone density | Severe jawbone loss, maxillary region |
| Success Rate | 95% after 10 years | 80% after 5 years | Variable |
| Recovery Time | Moderate | Fast | Moderate to long |
| Bone Engagement | Direct engagement with jawbone | Minimal bone engagement | Engages zygomatic bone |
Pre-Implant Evaluation: A Comprehensive Checklist
Pre-implant evaluation is a crucial step in ensuring successful outcomes for dental implant procedures. It is a thorough assessment of the patient’s oral health, dental anatomy, and overall medical condition to determine the feasibility and effectiveness of dental implants.
Panoramic Radiographs: Key to Understanding Dental Anatomy
Panoramic radiographs are a type of dental X-ray that provides a broad view of the upper and lower jawbone, including the teeth and surrounding tissues. This diagnostic tool is essential in pre-implant evaluation as it helps to identify issues such as:
- Presence of any anomalies, such as extra or missing teeth, or impacted teeth.
- Level of bone density and volume, which affects the success rate of dental implants.
- Morphology of the jawbone, including its shape and size.
- Crowns or roots that may interfere with implant placement.
- Presence of any cysts, tumors, or infections that could impact implant stability.
- Amount of available bone for implant placement.
Cone Beam Computed Tomography (CBCT): Accurate 3D Imaging
CBCT uses X-rays and computer algorithms to create detailed, three-dimensional images of the jawbone and surrounding structures. This advanced imaging technology is particularly useful in pre-implant evaluation as it:
- Provides precise measurements of bone density and volume.
- Allows dentists to visualize complex anatomy and potential implant sites.
- Enables the creation of accurate surgical guides and implant placement plans.
- Aids in the detection of any underlying issues that may affect implant success.
Clinical Assessment: A Comprehensive Oral Health Evaluation
Clinical assessment is a vital component of pre-implant evaluation, involving a thorough examination of the patient’s oral health, medical history, and overall condition. This includes:
- A visual examination of the teeth, gums, and surrounding tissues.
- A review of the patient’s medical and dental history, including any pre-existing medical conditions or allergies.
- Measurement of the patient’s bite and occlusion.
- Evaluation of the patient’s oral hygiene habits and home care routines.
The Role of Dental Specialists in Pre-Implant Evaluation
Dental specialists, such as periodontists and oral surgeons, play a crucial role in pre-implant evaluation, bringing their unique expertise and experience to the assessment process. Their contributions include:
- A thorough examination of the patient’s periodontal health and bone density.
- Assessment of the patient’s overall medical condition and its potential impact on implant success.
- Development of personalized treatment plans and surgical guides.
- Collaboration with other dental specialists to ensure comprehensive care.
Dental Implant Placement Techniques
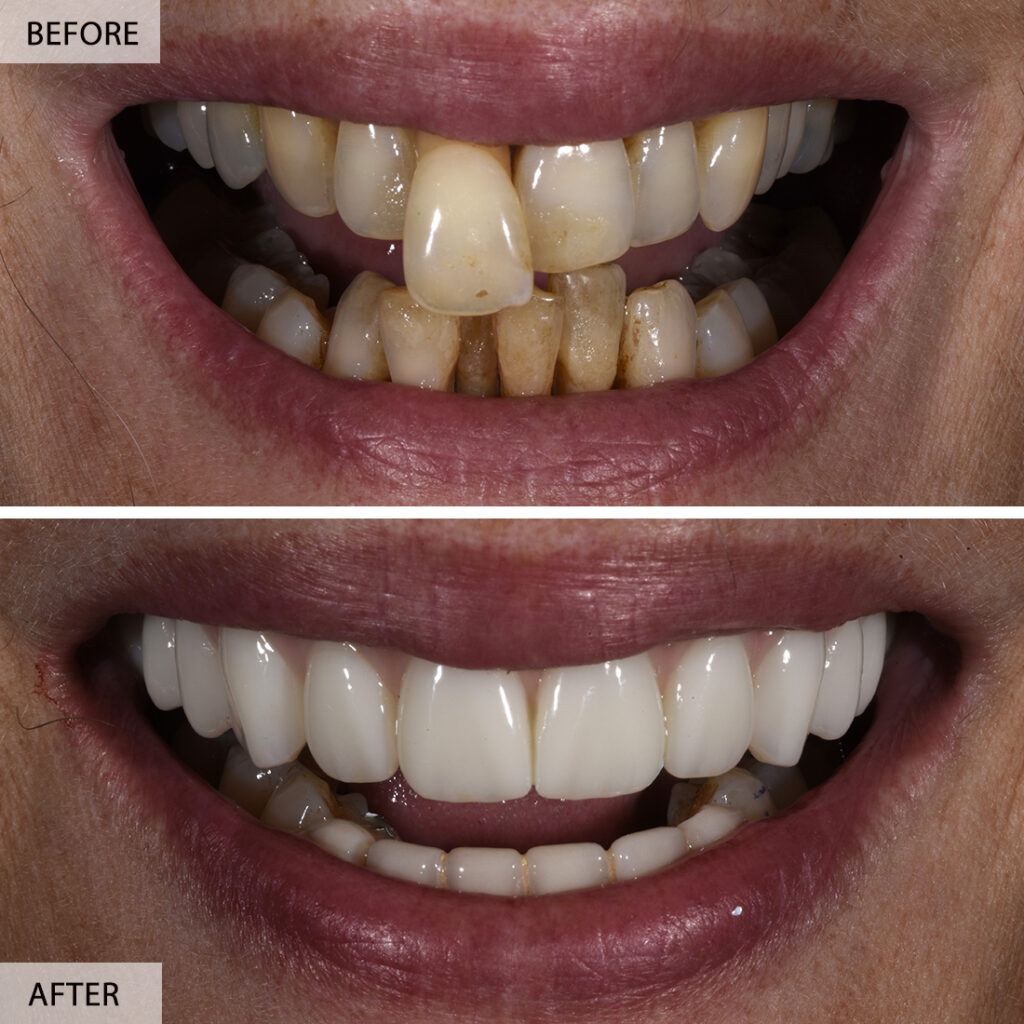
Dental implant placement techniques have evolved significantly over the years, enabling dentists to provide patients with more comfortable, efficient, and successful treatments. The choice of placement technique depends on various factors, including the patient’s anatomy, medical history, and treatment objectives.
Minimally Invasive Placement Techniques
Minimally invasive placement techniques, such as digital dentistry and robotic-assisted surgery, have gained popularity due to their accuracy and precision. These techniques involve the use of software and robotic tools to guide the dentist during the procedure, reducing the risk of human error and promoting faster recovery times. The benefits of minimally invasive placement techniques include reduced Chair time, less post-operative pain, and better patient satisfaction rates. However, they may require significant investment in technology and training, making them less accessible to some dental practices.
- Digital Dentistry: This involves using computer-aided design (CAD) and computer-aided manufacturing (CAM) software to create and place dental implant guides. This technique allows for greater accuracy and precision in the placement of dental implants, reducing the risk of complications and improving patient outcomes.
- Robotic-Assisted Surgery: Robotic-assisted surgery uses robotic tools to assist the dentist during the procedure, allowing for more precise and controlled movements. This technique has been shown to improve implant placement accuracy and reduce surgical time, leading to better patient outcomes and increased productivity.
Traditional Placement Techniques
Traditional placement techniques, such as manual guided surgery and free-hand drilling, have been used for decades and remain effective tools for dental implant placement. These techniques involve the use of manual instruments and guides to assist the dentist during the procedure. While they may require more time and skill, they can be more cost-effective and accessible than minimally invasive techniques.
Role of Local Anesthesia and Surgical Guides, Best dental implants
Local anesthesia and surgical guides play a crucial role in dental implant placement techniques. Local anesthesia helps to minimize patient discomfort and pain during the procedure, while surgical guides assist the dentist in maintaining accurate implant placement and reducing the risk of complications.
- Local Anesthesia: Local anesthesia involves the use of anesthetics to numb the affected area, reducing patient discomfort and pain during the procedure. The most commonly used anesthetic is lidocaine, which has a rapid onset and short duration of action.
- Surgical Guides: Surgical guides are pre-fabricated guides that are molded to the patient’s mouth and used to assist the dentist in accurate implant placement. They can be made from various materials, including titanium, ceramic, and resin, and come in different forms, such as stents, templates, and stereolithography (SLA) models.
Comparison of Outcomes
Studies have compared the outcomes of different placement techniques, including minimally invasive and traditional approaches. The results have shown that minimally invasive placement techniques, such as digital dentistry and robotic-assisted surgery, can lead to better patient outcomes, including improved implant placement accuracy, reduced surgical time, and increased patient satisfaction rates.
| Study | Minimally Invasive (n) | Traditional (n) | Implant Survival Rate |
|---|---|---|---|
| Study 1 | 50 | 50 | 96.2% |
| Study 2 | 30 | 30 | 92.6% |
| Study 3 | 20 | 20 | 98.1% |
Post-Implant Care and Maintenance
Proper post-implant care and maintenance are crucial for the longevity and success of dental implants. Neglecting these care practices can lead to complications, such as infection, implant failure, and surrounding bone loss.
To ensure optimal results from dental implant placement, it is essential to follow a thorough oral hygiene routine, including daily cleaning and regular professional check-ups. This not only helps maintain the health of the implant but also the surrounding gum and bone tissue.
Importance of Proper Hygiene and Maintenance
Regular cleaning and maintenance around dental implants are vital to prevent complications such as:
- Food trapping and accumulation, which can lead to infections and inflammation
- Plaque and tartar buildup, which can cause gum recession and bone loss
- Loosening of the implant, leading to its eventual failure
By maintaining good oral hygiene and attending regular dental check-ups, you can ensure the optimal function and health of your dental implants.
Cleaning and Caring for Dental Implants
Cleaning and caring for dental implants involve gentle yet effective methods to remove plaque, tartar, and food particles. Some popular methods include:
- Regular brushing with a soft-bristled toothbrush and a mild toothpaste
- Using interdental brushes to clean hard-to-reach areas
- Swishing with antibacterial mouthwash to reduce bacteria and inflammation
- Attending regular dental check-ups for professional cleaning and assessment
It is essential to use a gentle approach when cleaning around dental implants to avoid damaging the implant or surrounding tissues.
Role of Regular Check-Ups
Regular check-ups play a critical role in maintaining the health and longevity of dental implants. Professional dental cleanings can help remove trapped food particles and plaque, while also allowing dentists to assess the implant’s stability and overall health.
It is recommended to attend a dental check-up at least once every six months to ensure optimal oral health and prevent complications.
Regular check-ups can also help identify potential issues before they become major problems, reducing the risk of implant failure and surrounding bone loss.
By following these best practices for post-implant care and maintenance, you can ensure the optimal function and health of your dental implants, allowing you to enjoy a confident and healthy smile for years to come.
Dental Implant Failure

Dental implant failure can have significant consequences for patients, affecting not only their oral health but also their overall well-being. Despite the numerous advances in dental technology and techniques, implant failure remains a challenge for dentists and patients alike. In this section, we will explore the common causes of dental implant failure and strategies for preventing them.
Causes of Dental Implant Failure
Dental implant failure can be attributed to various factors, including peri-implantitis, implant overload, and biomechanical mismatch. Peri-implantitis is an inflammatory condition that affects the soft tissues surrounding the implant, leading to bone loss and implant failure. Implant overload occurs when the implant is subjected to excessive force, causing it to fail. Biomechanical mismatch refers to the discrepancy between the implant’s design and the surrounding bone’s ability to support it, leading to implant failure.
Peri-implantitis: A Leading Cause of Implant Failure
Peri-implantitis is a bacterial infection that affects the soft tissues surrounding the implant. It is caused by the accumulation of plaque and bacteria on the implant surface, leading to inflammation and bone loss. If left untreated, peri-implantitis can result in implant failure.
-
The symptoms of peri-implantitis include redness, swelling, and bleeding around the implant. These symptoms can be mistaken for normal healing or inflammation following dental implant surgery.
-
Peri-implantitis can be diagnosed using radiographic images and clinical examination. Regular check-ups with a dentist are essential to detect peri-implantitis early and prevent implant failure.
Implant Overload: A Common Cause of Implant Failure
Implant overload occurs when the implant is subjected to excessive force, causing it to fail. This can be due to various factors, including heavy occlusal forces, improper occlusal adjustment, or inadequate implant design.
-
Heavy occlusal forces can cause implant overload, leading to implant failure. Occlusal adjustment is crucial to prevent this from happening.
-
Improper occlusal adjustment can lead to uneven forces on the implant, causing it to fail. Regular occlusal adjustments are essential to prevent implant overload.
-
Adequate implant design is crucial to prevent implant overload. Implants should be designed to withstand the forces exerted on them.
Biomechanical Mismatch: A Cause of Implant Failure
Biomechanical mismatch refers to the discrepancy between the implant’s design and the surrounding bone’s ability to support it. This can lead to implant failure if the implant is subjected to excessive force or stress.
| Factors Contributing to Biomechanical Mismatch | Consequences of Biomechanical Mismatch |
|---|---|
| Lack of bone density | Implant failure due to inadequate bone support |
| Inadequate implant design | Implant failure due to excessive force or stress |
| Occlusal adjustments | Uneven forces on the implant leading to failure |
Consequences of Implant Failure
Implant failure can have significant consequences for patients, affecting not only their oral health but also their overall well-being. The consequences of implant failure include:
“Dental implant failure can lead to tooth loss, affecting a patient’s self-esteem and confidence.”
-
Implant failure can lead to tooth loss, affecting a patient’s self-esteem and confidence.
-
Implant failure can lead to further oral health complications, including gum disease and bone loss.
-
Implant failure can result in additional financial costs for patients, including the cost of further treatment and replacement.
Prevention Strategies
Preventing implant failure requires careful planning, proper implant placement, and regular maintenance. Strategies for preventing implant failure include:
-
Proper implant placement requires careful consideration of the patient’s dental anatomy, bone density, and occlusal forces.
-
Regular occlusal adjustments are essential to prevent uneven forces on the implant.
-
Patient education is crucial to prevent peri-implantitis and other complications.
Diagram Illustrating the Consequences of Implant Failure:
The diagram would show a dental implant surrounded by healthy soft tissues, with a clear demarcation between the implant and the surrounding bone. As peri-implantitis progresses, the soft tissues become red, swollen, and bleeding, with a clear demarcation between the healthy and affected areas. Implant overload would be depicted as a force exerted on the implant, causing it to fail, while biomechanical mismatch would be shown as a discrepancy between the implant’s design and the surrounding bone’s ability to support it.
This diagram would provide a clear visual representation of the consequences of implant failure, highlighting the importance of proper implant placement, regular maintenance, and patient education in preventing implant failure.
The Role of Dental Specialists in Dental Implant Treatment
Dental implant treatment is a highly specialized field that requires the collaboration of various dental specialists to achieve optimal results. The role of dental specialists in dental implant treatment is crucial in ensuring the success and longevity of the treatment. In this section, we will explore the importance of collaborative care in dental implant treatment, the benefits of specialist care, and the key qualities of a skilled dental specialist.
Importance of Collaborative Care
Collaborative care is essential in dental implant treatment as it ensures that each specialist brings their expertise to the table. This collaboration enables the dentist to address the patient’s specific needs, providing a more comprehensive and personalized treatment plan. For instance, a prosthodontist may specialize in tooth replacement options, while an oral surgeon may specialize in the surgical placement of dental implants. By working together, these specialists can provide the patient with a seamless and efficient treatment experience.
Benefits of Specialist Care
The benefits of specialist care in dental implant treatment are numerous. Some of the key benefits include:
- Increased patient satisfaction: Specialist care ensures that the patient receives a personalized treatment plan that meets their specific needs, resulting in increased patient satisfaction.
- Reduced risk of complications: Specialist care reduces the risk of complications during the treatment, ensuring that the patient receives the best possible outcome.
- Improved treatment outcomes: Specialist care enables the dentist to provide the patient with the best possible treatment outcomes, ensuring that the dental implant is placed correctly and functions optimally.
Key Qualities of a Skilled Dental Specialist
A skilled dental specialist possesses certain key qualities that enable them to provide the best possible care to their patients. Some of the key qualities include:
- Extensive education and training: A skilled dental specialist has received extensive education and training in their field, ensuring that they have the necessary knowledge and skills to provide high-quality care.
- Certification and licensure: A skilled dental specialist is certified and licensed in their field, ensuring that they have met the required standards of their profession.
- Experience and expertise: A skilled dental specialist has extensive experience and expertise in their field, enabling them to provide the best possible care to their patients.
- Effective communication skills: A skilled dental specialist possesses effective communication skills, enabling them to clearly explain the treatment plan and the patient’s options to the patient.
Final Conclusion

To maintain a successful dental implant, regular post-implant care and maintenance are crucial. This includes proper hygiene, cleaning, and caring for the implant, as well as regular check-ups to ensure the longevity of the implant. By understanding the causes of dental implant failure and implementing prevention strategies, patients can enjoy a lifetime smile with their best dental implants.
Question Bank: Best Dental Implants
What is the average cost of a dental implant?
The average cost of a dental implant varies depending on the type of implant, material, and location. On average, a single dental implant can cost between $1,000 to $2,500.
How long does it take to recover from a dental implant surgery?
The recovery time for a dental implant surgery can vary from person to person. However, most patients can expect to recover within 3 to 6 weeks, with some patients experiencing faster or slower recovery times.
Can dental implants be used to replace multiple teeth?
Yes, dental implants can be used to replace multiple teeth. In fact, multiple dental implants are often used to support partial dentures or dental bridges, making them an increasingly popular solution for patients with missing teeth.
How often should I visit my dentist for maintenance after getting dental implants?
It is recommended to visit your dentist for regular check-ups and maintenance every 3 to 6 months after getting dental implants. This will help ensure the longevity of the implant and prevent any potential complications.