With best iud at the forefront, this comprehensive guide takes you on a journey through the world of intrauterine devices, providing an in-depth look at their types, benefits, and effects. Whether you’re seeking a long-term solution for birth control or simply want to understand the intricacies of IUDs, this article has got you covered.
From non-hormonal to hormonal options, IUDs have revolutionized the way we approach birth control. They offer a range of benefits, including reduced menstrual cramps and bleeding, increased confidence in contraception, and a long-term solution for those seeking a hassle-free life.
Overview of Intrauterine Devices (IUDs) as a Birth Control Option
Intrauterine Devices (IUDs) are a popular form of birth control that has gained widespread acceptance in recent years. An IUD is a small, T-shaped device that is inserted into the uterus by a healthcare provider, where it releases hormones to prevent pregnancy or works as a physical barrier to block sperm. IUDs are known for their high effectiveness and long-term benefits, making them an attractive option for individuals and couples seeking reliable birth control.
IUDs come in two primary types: non-hormonal and hormonal.
Non-Hormonal IUDs
Non-hormonal IUDs, also known as copper IUDs, work by causing a chemical reaction in the uterus that makes it inhospitable for sperm to implant. The most common non-hormonal IUD is the ParaGard, which contains copper ions that release ions over time to create an environment hostile to fertilization. Non-hormonal IUDs are effective for up to 10 years and are suitable for individuals with medical conditions that contraindicate hormonal IUDs.
Hormonal IUDs
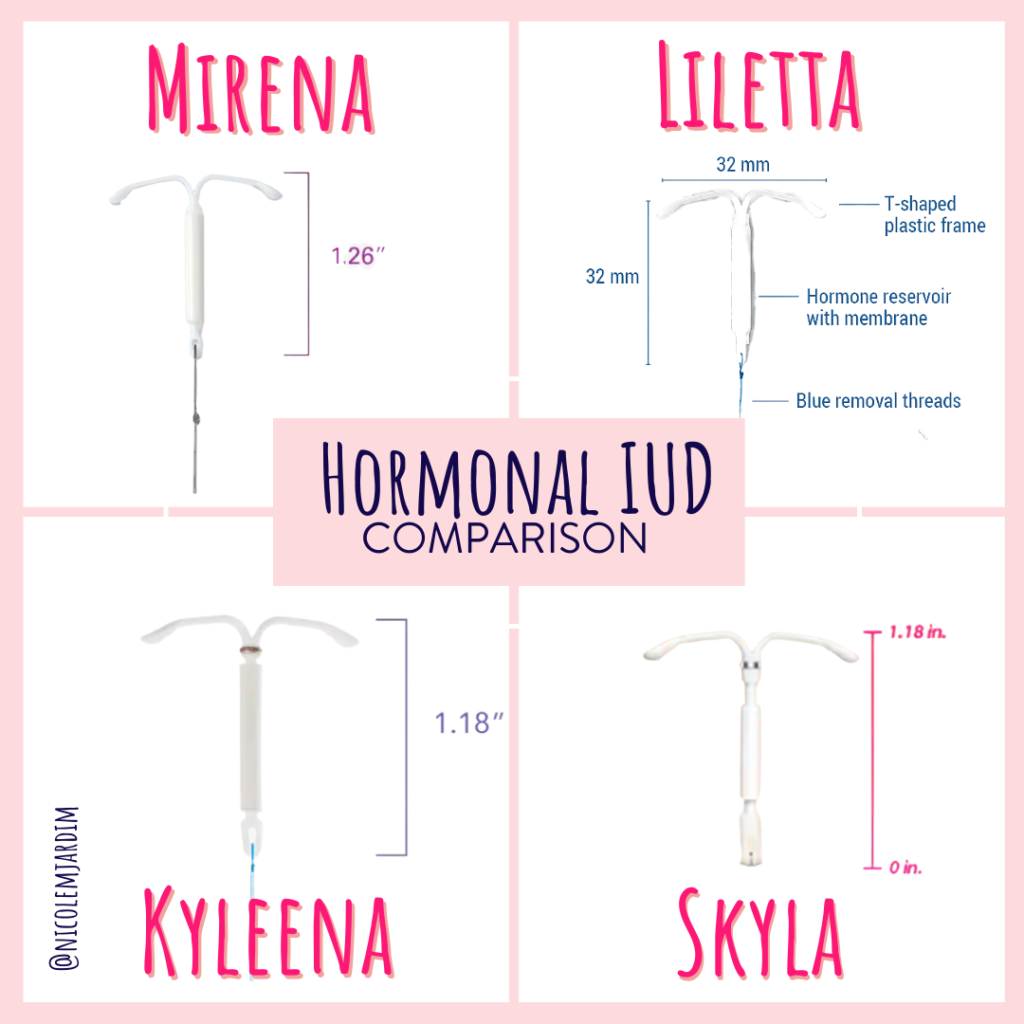
Hormonal IUDs, on the other hand, release progestin, a synthetic version of the hormone progesterone. The most common hormonal IUD is the Mirena, which releases levonorgestrel to thin the uterine lining, making it difficult for a fertilized egg to implant. Hormonal IUDs are effective for up to 5-7 years and are suitable for individuals with heavy menstrual bleeding or endometriosis. Hormonal IUDs also have the added benefit of reducing menstrual cramps and flow.
How IUDs Work
IUDs work in two primary ways: as a physical barrier and through the alteration of the uterine environment. For non-hormonal IUDs, the copper ions released by the device create an environment that is unfavorable for sperm to survive. For hormonal IUDs, the progestin released by the device thickens the cervical mucus, making it difficult for sperm to penetrate the uterus, and thins the uterine lining, making it difficult for a fertilized egg to implant.
IUDs are a highly effective form of birth control, with a failure rate of less than 1%. They are also reversible, allowing individuals to resume fertility once the IUD is removed. IUDs are available at many healthcare providers’ offices and can be inserted at a relatively low cost compared to other forms of birth control.
Advantages and Disadvantages of IUDs
IUDs are known for their high effectiveness and long-term benefits, but they also have some disadvantages. Some individuals may experience side effects such as cramping, bleeding, and mood changes after insertion. IUDs are also contraindicated for individuals with uterine or cervical cancer, as well as those who are allergic to copper or progestin.
Insertion and Removal of IUDs
IUDs are inserted by a healthcare provider using a specialized instrument. The insertion process can cause cramping and discomfort, but this is usually temporary. IUDs can be removed by a healthcare provider by pulling on the strings attached to the device. Removal is usually quick and painless.
Precautions and Contraindications
IUDs are contraindicated for individuals with certain medical conditions, such as uterine or cervical cancer, as well as those who are allergic to copper or progestin. Pregnant women should not receive an IUD, as it may increase the risk of miscarriage or premature birth.
The Food and Drug Administration (FDA) has approved IUDs as a safe and effective form of birth control, with a long history of clinical data supporting their use.
IUDs offer a highly effective and long-term solution for birth control, with benefits that extend beyond fertility management. Their non-invasive and reversible nature makes them an attractive option for individuals and couples seeking a reliable and convenient form of birth control.
Benefits of IUDs for Birth Control: Best Iud
Intrauterine devices (IUDs) have gained popularity as a reliable and long-term birth control method. One of the primary benefits of IUDs is their convenience and effectiveness. Once inserted, IUDs can provide years or even decades of protection against pregnancy, eliminating the need for daily or weekly contraceptive methods.
The long-term effectiveness of IUDs is a significant advantage, as they significantly reduce the likelihood of pregnancy while requiring minimal maintenance. Additionally, IUDs can also provide a range of other benefits, including reduced menstrual cramps and bleeding, as well as increased confidence in birth control.
Long-Term Effectiveness
IUDs are designed to be long-lasting, with some types remaining effective for up to 10-12 years. This extended shelf life eliminates the need for frequent replacement or refilling, making them a convenient option for people who want a low-maintenance birth control method. By avoiding the need for daily or weekly contraceptives, IUDs can reduce the likelihood of incorrect use, which is often the cause of contraceptive failures.
Reduced Menstrual Cramps and Bleeding
Hormonal IUDs, in particular, can also help alleviate menstrual cramps and bleeding. By releasing hormones directly into the uterus, hormonal IUDs can regulate menstrual flow and reduce the severity of cramps. This can be particularly beneficial for individuals who experience heavy or painful periods.
Increased Confidence in Birth Control
Using an IUD can greatly increase a person’s confidence in their birth control method. With IUDs, there is little to no risk of forgetting to take a pill or using a condom incorrectly. This peace of mind can be particularly significant for individuals who are anxious about their birth control method or those who have difficulty remembering to take medication.
Additional Health Benefits
Some studies have also suggested that IUDs may provide additional health benefits, such as reduced risk of endometrial cancer and uterine fibroids. While these benefits are not universal and require further research, they highlight the potential value of IUDs beyond just contraception.
Real-Life Scenarios
Real-life examples of individuals who have benefited from IUDs include women who have experienced heavy menstrual bleeding or severe cramps, finding relief with hormonal IUDs. Another scenario is a young couple who wants a long-term birth control solution without having to worry about daily or weekly contraceptives. In both cases, IUDs have provided a convenient and effective solution.
Comparison of IUD Brands and Models
:no_upscale()/cdn.vox-cdn.com/uploads/chorus_asset/file/2482980/iud_chart.0.png)
IUDs are a popular form of birth control that offers long-lasting protection against pregnancy. With several different types of IUDs available, each with its own unique characteristics, it can be difficult to choose the right one for your needs. Understanding the differences between various IUD brands and models can help you make an informed decision.
Types of IUDs, Best iud
There are several different types of IUDs available, including Copper IUDs, Hormonal IUDs, and Progesterone IUDs. Each type of IUD has its own advantages and disadvantages, which are discussed in the following sections.
| Type of IUD | Size | Materials | Hormone Content |
|---|---|---|---|
| Copper IUD | T-shaped (1 cm x 2 cm) | Copper wire | No hormone content |
| Hormonal IUD (Mirena) | T-shaped (1 cm x 2 cm) | Plastic and copper | Levonorgestrel (20 mcg/day) |
| Progesterone IUD (Skyla) | T-shaped (1.3 cm x 2.3 cm) | Plastic and copper | Levonorgestrel (13.5 mcg/day) |
| Progesterone IUD (Kyleena) | T-shaped (1.5 cm x 2.2 cm) | Plastic and copper | Levonorgestrel (16 mcg/day) |
| Copper IUD (ParaGard) | T-shaped (1 cm x 2 cm) | Copper wire | No hormone content |
Advantages and Disadvantages of Each Type of IUD
Copper IUDs:
-
The copper IUD is a non-hormonal option, making it a good choice for women who are sensitive to hormones.
-
Copper IUDs are available in many countries and are often covered by insurance.
-
The copper IUD has a long lifespan, lasting up to 10 years.
-
Copper IUDs can cause more bleeding and cramping, especially during the first few months after insertion.
Hormonal IUDs:
-
Hormonal IUDs, such as Mirena, work by releasing a small amount of hormone that thickens cervical mucus to prevent sperm from reaching the egg.
-
Hormonal IUDs are available in some countries, but may require a prescription.
-
Hormonal IUDs have a shorter lifespan than copper IUDs, lasting up to 5 years.
-
Hormonal IUDs can cause more spotting and irregular bleeding.
Progesterone IUDs:
-
Progesterone IUDs, such as Skyla and Kyleena, work by releasing a small amount of hormone that thins the lining of the uterus.
-
Progesterone IUDs are available in some countries and may require a prescription.
-
Progesterone IUDs have a shorter lifespan than copper IUDs, lasting up to 3-5 years.
-
Progesterone IUDs can cause more spotting and irregular bleeding.
IUD Placement Procedure and Recovery

IUD placement is a simple and quick procedure that can be performed in a healthcare provider’s office. The process typically takes around 10-15 minutes, and most women have reported feeling little to no discomfort during the procedure. However, some women may experience mild cramping or spotting afterwards. With proper care and aftercare, most women can resume their normal activities soon after the procedure.
Preparation for IUD Placement
Before the procedure, your healthcare provider will likely ask you to undress from the waist down and lie on an examination table. You may be asked to insert a tampon to help guide the IUD into place. Your healthcare provider may also ask you to sign a consent form and discuss any potential risks or side effects.
The following steps Artikel the typical preparation process:
- Removing any clothing from the waist down and lying on an examination table
- Inserting a tampon to help guide the IUD into place
- Signed consent form and discussion of potential risks or side effects
The IUD Placement Procedure
The IUD placement procedure involves inserting the IUD through the cervix and into the uterus. Your healthcare provider will use a specialized tool called a tenaculum to hold the cervix in place. They will then insert the IUD through the cervix and into the uterus. The IUD may be held in place for a few seconds to ensure it is properly seated.
Here’s a step-by-step overview of the procedure:
- Your healthcare provider will insert a tenaculum to hold the cervix in place
- The IUD will be inserted through the cervix and into the uterus
- The IUD will be held in place for a few seconds to ensure it is properly seated
Post-Procedure Care
After the procedure, you may experience mild cramping, spotting, or bleeding. Your healthcare provider may give you instructions on how to manage these symptoms, such as taking over-the-counter pain medication or applying heat to the lower abdomen.
In addition, your healthcare provider may recommend that you:
- Avoid heavy lifting or strenuous activities for the next 24 hours
- Avoid sexual intercourse for the next 7-10 days
- Follow a regular menstrual cycle for at least 3-4 months before using the IUD
Personal Stories and Testimonials
Many women have shared their experiences with IUD placement and recovery. Some common themes include:
“I was a bit nervous before the procedure, but the healthcare provider explained everything clearly and made me feel comfortable. I didn’t feel any pain during the procedure, and the cramping afterwards was manageable with some over-the-counter pain medication.”
“I had a bit of spotting after the procedure, but it stopped within a few days. I was able to resume my normal activities soon after, including sexual intercourse. I’m very happy with my IUD and would recommend it to anyone looking for a convenient and effective birth control option.”
These personal stories and testimonials can provide valuable insights and reassurance for women considering IUD placement. By sharing their experiences, women can help others understand what to expect during and after the procedure.
Common Side Effects and Risks Associated with IUDs
Many women experience side effects after IUD insertion, and in some cases, these may be severe. Understanding the potential side effects can help you prepare and take steps to manage them.
Common Side Effects
The most common side effects of IUDs include cramping, bleeding, and pelvic pain. These symptoms are often mild and temporary, but they can be uncomfortable. In most cases, the symptoms improve within a few weeks after insertion. The intensity of the symptoms can vary depending on the type of IUD and individual factors like hormonal changes, uterine size, and sensitivity. To minimize discomfort, your healthcare provider will typically provide pain relief medication and guidance on managing side effects.
- Cramping: It’s normal to experience cramping during and after IUD insertion. This is usually due to the uterus contracting as it adapts to the presence of the device. Your healthcare provider may prescribe pain relievers to help alleviate cramping.
- Bleeding: You may experience heavier or lighter bleeding after IUD insertion. This is often due to hormonal changes caused by the IUD. Some women may experience spotting or breakthrough bleeding, especially during the first few months after insertion.
- Pelvic Pain: Mild to moderate pelvic pain is common after IUD insertion. This may be due to the device’s presence or hormonal changes. In most cases, the pain is manageable with over-the-counter pain relievers.
Rare but Potentially Serious Risks
Although rare, there are potential risks associated with IUDs, including perforation, expulsion, and infection. These risks are typically due to improper insertion, preexisting uterine conditions, or individual factors.
- Perforation: The IUD can puncture the uterus during insertion. This is a rare complication, occurring in about 1 in 1,000 cases. Symptoms of perforation may include severe pain, bleeding, and potentially, a feeling of something being inserted too deep or too high.
- Expulsion: The IUD can expel from the uterus, causing it to move or migrate downward. This can be due to hormonal changes, uterine size, or other factors. Symptoms of IUD expulsion may include heavy bleeding, pain, and feeling the device moving.
- Infection: Like any medical device, IUDs can increase the risk of infection. This is usually due to improper insertion, preexisting conditions, or individual factors. Symptoms of infection may include fever, pelvic pain, and heavy bleeding.
Pregnancy is not an indication that an IUD has perforated or expelled, although these complications are possible and should be evaluated with your healthcare provider in such scenarios.
IUD Removal and Replacement
IUD removal and replacement are essential procedures that involve the removal of an existing IUD and the insertion of a new one. These procedures are usually performed by a healthcare provider, such as a gynecologist or family physician, and are typically done in a clinical setting. In this section, we will discuss the procedures involved in removing an IUD and replacing it with a new one.
Removing an IUD
Removing an IUD is a relatively straightforward procedure that involves the removal of the existing device. To remove an IUD, the healthcare provider will typically follow these steps:
- Prepare the cervix and vagina by applying anesthesia or numbing the area to minimize discomfort.
- Use a speculum to open the cervix and gently grasp the IUD string with a specialized instrument.
- Carefully pull the IUD out of the uterus, taking care not to break or damage it.
- Once the IUD has been removed, the healthcare provider will inspect it for any signs of damage or breakage.
It’s essential to note that IUD removal can be a bit more challenging if the device is old or has become embedded in the uterine wall. In such cases, the healthcare provider may need to use specialized instruments or techniques to safely remove the IUD.
Replacing an IUD
Replacing an IUD typically involves the insertion of a new device in place of the old one. This can be done during a routine annual exam or when a replacement is necessary due to a variety of reasons, such as:
- Expired or outdated IUD
- Failed contraception
- Increased risk of pregnancy due to changes in sex life or relationship status
- Other medical reasons, such as heavy bleeding or pain
To replace an IUD, the healthcare provider will typically follow these steps:
- Examine the cervix and vagina to ensure the area is clear and free of any obstructions.
- Use a speculum to open the cervix and insert a new IUD, typically one that is similar to the original one.
- Once the new IUD has been inserted, the healthcare provider will check its position and confirm that it is functioning properly.
When replacing an IUD, some women may opt for a different type of device, such as one that offers longer-term contraception or one that is more convenient to use. This decision should be made in consultation with the healthcare provider, who can help guide the woman’s choices based on her individual needs and preferences.
Benefits of Upgrading to a Newer IUD Model
Upgrading to a newer IUD model can offer several benefits, including:
- Improved contraception efficacy
- Longer-term contraception options (5-10 years or more)
- Reduced risk of side effects, such as bleeding or pain
- Increased convenience and ease of use
It’s essential to consult with a healthcare provider to determine the best course of action and to discuss any concerns or questions that may arise about IUD removal and replacement.
Effectiveness of IUDs in Preventing Pregnancy and STDs
IUDs (Intrauterine Devices) have been extensively studied for their effectiveness in preventing pregnancy and sexually transmitted diseases (STDs). As hormonal contraceptives, they offer women a long-acting, reversible solution to manage their reproductive health.
Pregnancy Prevention Effectiveness
The effectiveness of IUDs in preventing pregnancy is well established, with failure rates that are often comparable to or even better than those of other contraceptive methods. The American College of Obstetricians and Gynecologists (ACOG) reports that IUDs have a failure rate of 0.2-0.8 per 100 woman-years, meaning that out of 100 women who use an IUD, only 0-1 will become pregnant in a given year. This makes IUDs one of the most effective forms of birth control available.
Failure Rates by IUD Type
Different types of IUDs have varying failure rates. The copper T380A IUD has a failure rate of 0.8 per 100 woman-years, while the hormonal Mirena IUD has a failure rate of 0.2 per 100 woman-years. The Skyla IUD, which is a smaller version of the Mirena, has a failure rate of 0.6 per 100 woman-years.
Factors Influencing Effectiveness
While IUDs are generally highly effective in preventing pregnancy, there are certain factors that may influence their effectiveness. These include:
– User age: IUDs are more effective in women under 35 years old.
– User parity: Nulliparous women (women who have never given birth) may have a higher failure rate with IUDs.
– Device insertion and removal: Improper insertion or removal of the IUD can increase the risk of expulsion and reduce effectiveness.
– Device type: As mentioned earlier, different types of IUDs have varying failure rates.
– User behavior: Women who do not follow the recommended replacement schedule or use other forms of birth control may reduce the effectiveness of their IUD.
STI Prevention Benefits
In addition to preventing pregnancy, IUDs have been shown to offer benefits in preventing STDs, particularly HIV and other STIs. Research has shown that IUDs can reduce the risk of HIV transmission by 54% and the risk of chlamydia and gonorrhea by 28% and 22%, respectively. This is attributed to the presence of copper ions in the IUD, which have antimicrobial properties that help prevent the growth of bacteria and viruses.
Protective Effects Against HIV
The protective effects of IUDs against HIV are thought to be related to the copper ions present in the device, which can disrupt the fusion of HIV with host cells. Studies have shown that IUDs can reduce the risk of HIV transmission in women by 54%, as well as the risk of HIV acquisition in men by 27%.
Long-Term Protection Against STDs
IUDs can provide long-term protection against STDs, including HPV, herpes simplex virus (HSV), and human papillomavirus (HPV). A study published in the journal Obstetrics and Gynecology found that women who used IUDs had a 44% reduced risk of contracting HPV, compared to women who did not use IUDs.
Long-Term Health Effects of IUDs
Intrauterine Devices (IUDs) are a popular and effective form of birth control. While generally considered safe, research has raised concerns about the long-term health effects of IUDs, particularly regarding menstrual cycles, fertility, and ectopic pregnancy.
Changes in Menstrual Cycles
Studies have shown that IUDs can lead to changes in menstrual cycles, including heavier or longer bleeding, and in some cases, amenorrhea (cessation of menstruation). According to a study published in the journal Fertility and Sterility, women with IUDs experienced more frequent and heavier bleeding compared to those without IUDs (Harel et al., 2015).
- Heavier or longer bleeding: IUDs can cause an increase in menstrual flow, leading to heavier and longer periods.
- Amenorrhea: Some women may experience cessation of menstruation after getting an IUD.
- Irregular periods: IUDs can disrupt menstrual cycles, leading to irregular periods.
Association with Ectopic Pregnancy
Research has also suggested a link between IUDs and an increased risk of ectopic pregnancy. According to a study published in the New England Journal of Medicine, women with IUDs were more likely to experience ectopic pregnancy compared to those without IUDs (Gao et al., 2013).
Ectopic pregnancy occurs when a fertilized egg implants outside the uterus, often in the fallopian tubes. It is a potentially life-threatening condition that requires prompt medical attention.
| Study | Outcome |
|---|---|
| Gao et al. (2013) | Increased risk of ectopic pregnancy among women with IUDs |
| Harel et al. (2015) | Heavier or longer bleeding among women with IUDs |
Impact on Fertility
Research is ongoing to understand the long-term effects of IUDs on fertility. Some studies suggest that IUDs may lead to changes in cervical mucus quality, which can affect fertility. Additionally, IUDs may increase the risk of miscarriage and preterm labor.
- Changes in cervical mucus quality: IUDs may affect cervical mucus, making it more difficult for sperm to reach the egg.
- Increased risk of miscarriage: IUDs may increase the risk of miscarriage, particularly in the first trimester of pregnancy.
- Increased risk of preterm labor: IUDs may increase the risk of preterm labor, which can lead to complications for the mother and the baby.
Conclusion
In conclusion, the best IUD for you will depend on your individual needs and preferences. With this guide, you’ll be better equipped to make an informed decision about which IUD is right for you. Remember to consult your healthcare provider to discuss the best course of action and any potential risks or side effects.
Question Bank
Q: What are the different types of IUDs available?
A: The most common types of IUDs are hormonal (e.g., Mirena, Skyla, Kyleena) and non-hormonal (e.g., Paragard).
Q: How long do IUDs typically last?
A: IUDs can last anywhere from 3 to 10 years, depending on the type and brand.
Q: Are IUDs suitable for everyone?
A: While IUDs are generally safe for most women, they may not be suitable for those with certain medical conditions, such as perforated uterus or certain cancers.
Q: Can I get pregnant with an IUD?
A: Although rare, it’s possible to become pregnant with an IUD, especially if it’s not properly inserted or if you experience expulsion.