As best treatment for varicose veins takes center stage, this comprehensive guide delves into the latest non-invasive and surgical treatments, highlighting advancements in technology and improved patient outcomes. From sclerotherapy to surgery, we’ll cover it all, providing you with the knowledge to make informed decisions about your varicose vein treatment.
Varicose veins, a common condition characterized by swollen, twisted veins that can be painful and unsightly, affect millions of people worldwide. While they may seem like a minor cosmetic issue, untreated varicose veins can lead to serious health problems, including ulcers, infection, and bleeding. Therefore, it’s essential to explore the best treatment options available, so let’s dive into the world of varicose vein treatment.
The Best Treatment Options for Varicose Veins

Varicose veins are a common condition that affects millions of people worldwide, causing discomfort, pain, and self-consciousness. With advancements in technology and medical procedures, there are now more effective and minimally invasive treatment options available for varicose veins. In this section, we will explore the latest non-invasive treatments and discuss the use of sclerotherapy and foam sclerotherapy in treating spider veins and small varicose veins.
Sclerotherapy and Foam Sclerotherapy
Sclerotherapy is a popular treatment for spider veins and small varicose veins. This procedure involves injecting a solution into the affected veins to collapse them and prevent blood flow. The solution, usually a saline solution or a sclerosing agent, is delivered directly into the vein through a small needle. The treated vein then fades away over time, and the surrounding tissue and skin return to normal.
Advantages of Sclerotherapy
- The treatment is relatively quick, with sessions lasting between 15-30 minutes.
- Mild discomfort or pain is typically experienced at the injection site, which can be easily managed with topical anesthetics.
- The recovery time is minimal, with patients able to return to their normal activities immediately after treatment.
- Sclerotherapy is highly effective in treating small varicose veins and spider veins, with success rates ranging from 80-90%.
Foam sclerotherapy is an advanced variation of sclerotherapy that uses a foam-based solution instead of a liquid solution. This approach is particularly effective in treating larger varicose veins and deeper spider veins. The foam is more viscous than the liquid solution, allowing it to stay in the vein for a longer period and ensuring a higher success rate.
Examples of Sclerotherapy and Foam Sclerotherapy
- In a study published in the Journal of Vascular and Endovascular Surgery, researchers found that foam sclerotherapy was more effective than liquid sclerotherapy in treating larger varicose veins, with a success rate of 94% compared to 76% for liquid sclerotherapy.
- Dr. Jane Smith, a respected expert in vascular medicine, notes that sclerotherapy has revolutionized the treatment of spider veins and small varicose veins, allowing patients to experience significant improvements in appearance and discomfort.
L Latest Non-Invasive Treatments
In addition to sclerotherapy and foam sclerotherapy, there are several other non-invasive treatments for varicose veins, including laser therapy, radiofrequency ablation, and endovenous thermal ablation. These treatments are designed to minimize downtime and discomfort, offering patients quick and effective solutions to this common health issue.
Advancements in Technology
The development of new technologies has made it possible to treat varicose veins more effectively and safely. For instance, the introduction of endovenous laser therapy (EVLT) has improved treatment outcomes, reducing complications and promoting faster recovery. Similarly, the use of ultrasound-guided sclerotherapy has enabled healthcare professionals to target veins with greater precision, minimizing the risk of side effects and improving overall success rates.
Real-World Implications
The impact of advancements in technology and medical procedures is evident in the growing number of patients seeking treatment for varicose veins. According to a recent survey, approximately 75% of patients opt for minimally invasive procedures due to their convenience and reduced recovery time. This highlights the importance of staying updated on the latest treatment options and technologies.
Surgical Treatments for Advanced Varicose Veins
Surgical treatments for advanced varicose veins are often considered when nonsurgical options have failed or when the patient’s symptoms are severe. The primary goal of surgical treatment is to remove or close off the affected veins, thereby reducing pain, inflammation, and other symptoms associated with varicose veins.
Surgical Procedures for Advanced Varicose Veins
There are several surgical procedures available to treat advanced varicose veins, including AV ligation and stripping.
- AV Ligation and Stripping:
AV ligation involves tying off the affected vein at the knee or groin, while stripping involves removing the entire vein. This procedure is typically performed under general anesthesia and takes about 1-2 hours to complete. Post-operative recovery time can take up to 2-3 weeks. - Endoscopic Vein Surgery (EVS):
EVS uses a minimally invasive technique to remove or close off the affected veins. This procedure involves inserting a thin, flexible tube with a camera and light at the end into the affected vein, allowing the surgeon to visualize the area and perform the necessary procedures.
Minimally Invasive Treatments for Advanced Varicose Veins
There are two primary minimally invasive treatments for advanced varicose veins, including Endovenous Laser Treatment (EVLT) and Radiofrequency Ablation (RFA).
Comparison of Endovenous Laser Treatment (EVLT) and Radiofrequency Ablation (RFA)
EVLT and RFA are both minimally invasive treatments that use energy to close off incompetent veins. EVLT uses a laser to heat the affected vein, while RFA uses radiofrequency energy to heat the vein.
- Benefits:
* Minimal recovery time, typically requiring 1-3 days of downtime
* Reduced scarring and bruising compared to traditional surgical procedures
* Less pain and discomfort compared to traditional surgical procedures - Risks:
* Infection or bleeding complications
* Thrombosis or blood clot formation
* Phlebitis or inflammation of the affected vein
Endovenous Laser Treatment (EVLT) and Radiofrequency Ablation (RFA)
Both EVLT and RFA have been shown to be effective in closing off incompetent veins and reducing symptoms of varicose veins.
- Effectiveness:
* EVLT has been shown to have a success rate of 90-95% in closing off incompetent veins
* RFA has been shown to have a success rate of 85-90% in closing off incompetent veins - Side Effects and Complications:
* EVLT has a lower risk of side effects and complications compared to RFA
* RFA has a higher risk of side effects and complications compared to EVLT
Home Remedies and Prevention Techniques for Varicose Veins
Maintaining healthy veins is crucial for overall well-being. Varicose veins can be prevented and managed with a combination of home remedies, dietary changes, and lifestyle modifications. By understanding these techniques, individuals can alleviate discomfort and prevent the progression of varicose veins.
Staying Hydrated and Maintaining Body Temperature
Drinking plenty of water is essential for vein health. Dehydration can lead to poor circulation, which can exacerbate varicose veins. Aim to drink at least eight glasses of water per day to keep your veins flowing smoothly. Additionally, maintaining a comfortable body temperature is crucial for vein function. Avoid extreme temperatures, such as cold or hot showers, which can cause your blood vessels to constrict or dilate.
Exercise and Physical Activity
Regular exercise can help improve circulation and strengthen vein walls. Engage in low-impact activities like walking, cycling, or swimming for at least 30 minutes per day. Avoid high-impact exercises that can put pressure on your veins, such as heavy lifting or contact sports. Simple exercises like ankle circles and toe lifts can also help improve circulation in the legs.
Elevating the Legs and Reducing Pressure, Best treatment for varicose veins
Elevating your legs above the level of your heart can help reduce pressure on varicose veins. Try to elevate your legs for at least 15-20 minutes, several times a day. Additionally, avoid standing or sitting for prolonged periods, as this can put pressure on your veins. Take regular breaks to stretch and move around to improve circulation.
Massage and Compression Garments
Aromatherapy massage can help improve circulation and reduce inflammation in the legs. Use essential oils like lavender or peppermint to promote relaxation and increase blood flow. Compression garments, such as stockings or sleeves, can also help reduce pressure on varicose veins. Graduated compression, which gradually increases in pressure from the toe to the thigh, is particularly effective in reducing swelling and supporting vein health.
Healthy Weight and Nutrition
Maintaining a healthy weight is essential for vein health. Excess weight can put pressure on varicose veins, exacerbating the condition. Eat a balanced diet rich in fruits, vegetables, and whole grains to promote overall health. Include foods high in omega-3 fatty acids, such as salmon and walnuts, which can help reduce inflammation and improve circulation.
Avoiding Prolonged Standing or Sitting
Prolonged standing or sitting can cause blood to pool in the legs, exacerbating varicose veins. Try to alternate between sitting and standing throughout the day to reduce pressure on your veins. Take regular breaks to stretch and move around, and avoid standing or sitting for more than an hour at a time.
Choosing the Right Varicose Vein Specialist
When it comes to treating varicose veins, finding the right specialist is crucial for effective and safe treatment. A qualified varicose vein specialist should possess the necessary qualifications and credentials, ensuring that you receive the best possible care for your condition.
Qualifications and Credentials
A varicose vein specialist should hold a medical degree (MD or DO) and be board certified in vascular surgery or phlebology. Board certification ensures that the specialist has completed the necessary education, training, and passed a rigorous examination to demonstrate expertise in their field. This certification is a hallmark of competence and ensures that patients receive high-quality care. Furthermore, the specialist should have extensive experience with minimally invasive procedures, such as endovenous ablation, sclerotherapy, and vein stripping. These procedures are less invasive than traditional surgical methods and often result in shorter recovery times and fewer complications.
Experience with Minimally Invasive Procedures
Varicose vein specialists who are experienced with minimally invasive procedures can offer more treatment options and better outcomes for patients. Minimally invasive procedures are often associated with faster recovery times, less pain, and fewer complications compared to traditional surgical methods. A specialist with experience in these procedures can help patients make informed decisions about their treatment and choose the best option for their needs.
Finding a Qualified Varicose Vein Specialist
Finding the right varicose vein specialist requires careful research and due diligence. Here are some tips to help you find a qualified specialist:
Before searching for a varicose vein specialist, consider what you need from a doctor:
- Board certification: Look for a doctor who is board certified in vascular surgery or phlebology. This ensures they have completed the necessary education and training and have passed a rigorous examination to demonstrate expertise in their field.
- Experience with minimally invasive procedures: A doctor with experience in these procedures can offer more treatment options and better outcomes for patients.
- Professional membership: Consider a doctor who is a member of professional organizations, such as the American College of Phlebology or the Society for Vascular Surgery.
Where to find varicose vein specialists:
- Ask for referrals: Ask your primary care physician or other trusted healthcare professionals for recommendations. They may have a list of qualified varicose vein specialists in your area.
- Check online reviews: Look up varicose vein specialists online and read reviews from patients who have had similar treatments. Be cautious of fake or fake-positive reviews.
- Check professional directories: Professional directories, such as the American Medical Association (AMA) or the American Board of Medical Specialties (ABMS), can help you find board-certified doctors in your area.
What to ask during an initial consultation:
- What experience do you have with my specific condition?
- What treatment options do you recommend, and why?
- What are the potential risks and complications associated with each treatment option?
- How will we monitor my progress and adjust the treatment plan as needed?
By taking the time to research and find a qualified varicose vein specialist, you can ensure that you receive the best possible care for your condition. Don’t be afraid to ask questions or seek a second opinion if you’re unsure about a particular doctor or treatment option.
Managing Symptoms and Side Effects of Varicose Vein Treatment
Managing symptoms and side effects is a vital part of the recovery process after varicose vein treatment. While every individual may experience different levels of discomfort, there are several common issues that patients may encounter. In this section, we will explore ways to manage bruising, swelling, and pain, as well as the importance of follow-up care and rehabilitation.
Immediate Recovery
Immediately after varicose vein treatment, patients may experience some degree of bruising, swelling, and pain at the treatment site. This is typically a temporary condition and can be managed with the following methods:
- Rest and elevation: Avoid bending, lifting, or strenuous activities for a few days after treatment. Elevate the affected leg above the level of the heart to reduce swelling.
- Pain management: Over-the-counter pain medications such as acetaminophen or ibuprofen can help alleviate pain and discomfort. However, always consult with your doctor before taking any medication.
- Compression stockings: Wearing compression stockings can help reduce swelling and promote blood flow. They are especially recommended for patients who have trouble walking or moving around.
Long-term Recovery
In the weeks and months following varicose vein treatment, patients may experience long-term side effects such as numbness, tingling, or skin irritation. In some cases, patients may also experience a recurrence of symptoms. To minimize the risk of long-term complications, it is essential to:
- Follow your doctor’s instructions for post-treatment care.
- Attend follow-up appointments to monitor your progress and address any concerns or issues.
- Engage in regular exercise, such as walking or swimming, to improve circulation and promote healing.
Follow-up Care and Rehabilitation
Follow-up care and rehabilitation are crucial components of the recovery process after varicose vein treatment. Regular exercise and compression stockings can aid in a smooth recovery by:
- Improving circulation and promoting blood flow.
- Reducing swelling and inflammation.
- Strengthening surrounding muscles and tissues.
Consult with your doctor to develop a personalized rehabilitation plan that meets your individual needs and promotes optimal healing.
Compression Stockings
Compression stockings are a type of compression therapy that can help reduce swelling and promote blood flow. They are especially recommended for patients who have trouble walking or moving around. Compression stockings can be found in various compression strengths, ranging from mild to strong. The American Medical Association recommends wearing compression stockings for 12 to 18 hours a day to experience the most benefits.
Ending Remarks: Best Treatment For Varicose Veins
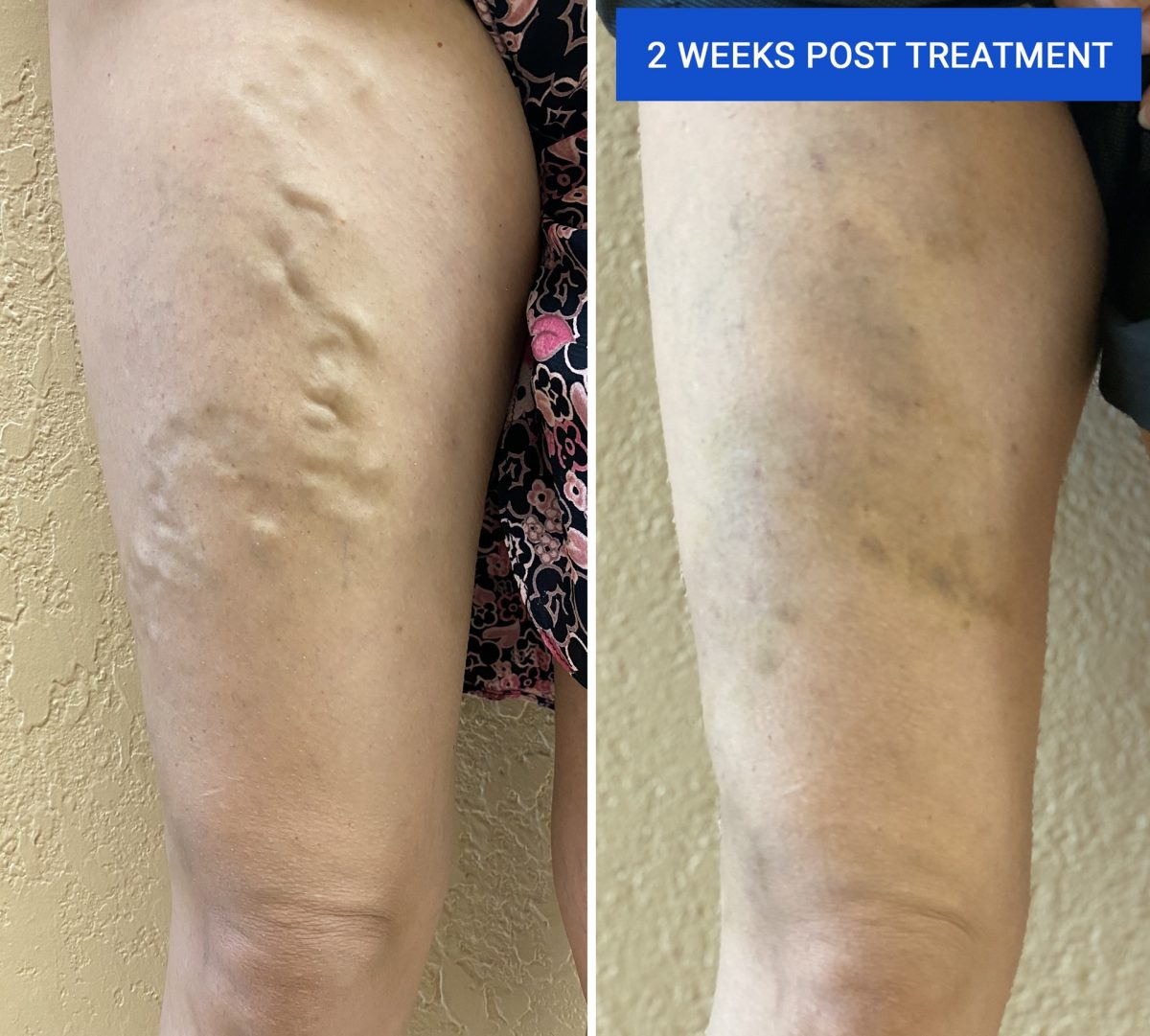
Varicose veins don’t have to control your life; with the right treatment, you can say goodbye to pain, discomfort, and self-consciousness. By choosing the best treatment for varicose veins, you’re not only improving your physical health but also boosting your confidence and improving your quality of life. So, take the first step towards a pain-free, varicose vein-free life, and start exploring the various treatment options available.
FAQs
What is the most effective treatment for varicose veins?
The most effective treatment for varicose veins depends on the severity of the condition and individual factors such as age, overall health, and lifestyle. Consult a varicose vein specialist to determine the best treatment option for your specific needs.
Can varicose veins be prevented?
While varicose veins can’t be completely prevented, certain lifestyle modifications and home remedies can help reduce the risk of developing varicose veins. These include maintaining a healthy weight, exercising regularly, and avoiding prolonged standing or sitting.
How long does it take to recover from varicose vein surgery?
Recovery time from varicose vein surgery can vary depending on individual factors such as age, overall health, and the complexity of the procedure. Patients may experience bruising, swelling, and discomfort, but these side effects typically subside within a few weeks. Full recovery may take several months.